Table of Contents
A newly licensed therapist waited four months after joining a group practice before her first insurance claim paid. Not because she wasn’t qualified. Because one document in her CAQH profile was uploaded in the wrong format and flagged , silently , by the payer. No one followed up. No one noticed. Four months of sessions billed at out-of-pocket rates instead of in-network reimbursement.
That scenario , a small documentation error creating a long, expensive delay , is the most common credentialing story in behavioral health. This guide is designed to prevent it.
What Is Behavioral Health Credentialing and Why Do Delays Cost So Much?
Behavioral health credentialing is the process by which insurance payers verify a provider’s qualifications, licenses, and practice information before granting in-network billing status. Until a provider is credentialed, they cannot bill as in-network , meaning the practice absorbs the difference in reimbursement or bills patients at full out-of-pocket rates.
The revenue math is clear: a therapist billing $5,000/month in-network generates nothing in-network reimbursement during a credentialing gap. A 90-day delay is $15,000 in unbilled insurance revenue , per provider. For a group practice adding three clinicians simultaneously, that’s $45,000.
Credentialing doesn’t just take time. It takes time proportional to how well it was prepared.
Every Month You're Not Credentialed Is a Month You're Not Getting Paid In-Network.
Credentialing delays cost behavioral health providers thousands in unbillable revenue. BehavioralProz manages the entire process , documents, applications, payer follow-up , so you can start seeing patients at in-network rates as fast as possible.
What Are the Universal Documents Every Behavioral Health Provider Needs?
Regardless of specialty, every provider credentialing with commercial payers needs:
- ✅ National Provider Identifier (NPI) , Individual Type 1 NPI confirmed active
- ✅ CAQH ProView profile , Completed, attested, and marked as “authorize” for target payers
- ✅ Current state license , Copy uploaded; confirm expiration date is future-dated
- ✅ DEA certificate (if applicable) , Required for prescribers; some payers require it for all MDs/DOs
- ✅ Malpractice insurance certificate , With $1M/$3M or payer-required limits; must show retroactive coverage dates
- ✅ CV or work history , Covering the last 5–10 years with no unexplained gaps
- ✅ Education and training documents , Diplomas, transcripts, residency completion letters
- ✅ Board certification (if applicable) , Current and verified
- ✅ W-9 , For tax identification
- ✅ Signed payer-specific credentialing application
These are the floor. Every specialty adds requirements on top of this.
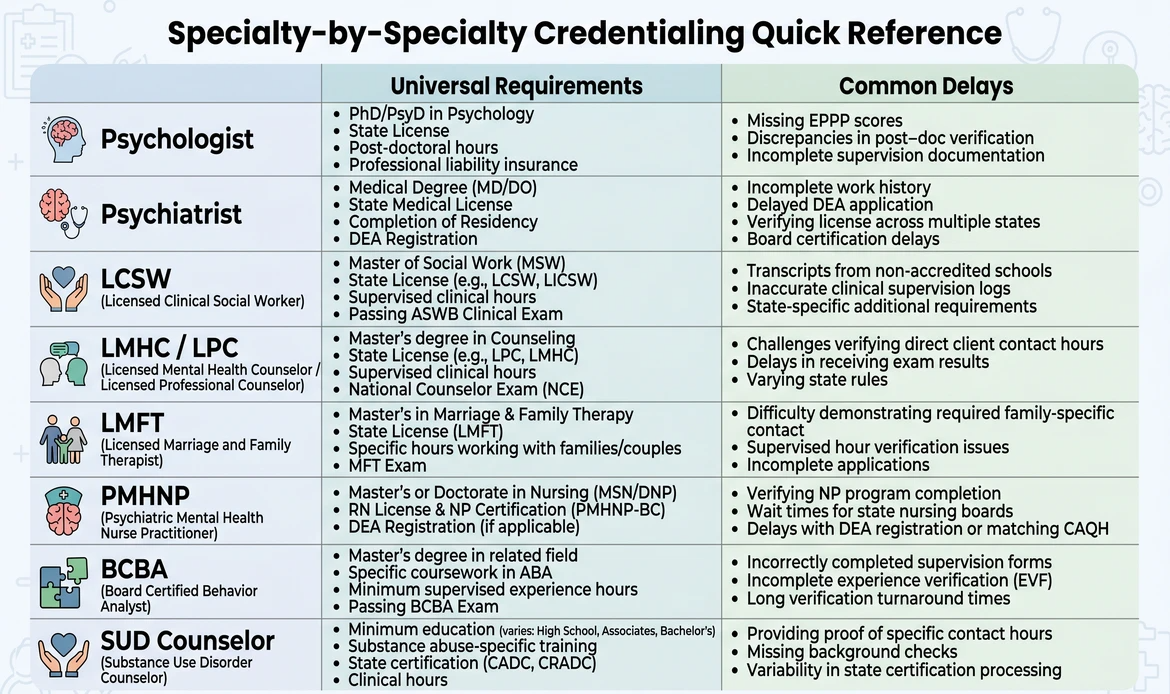
What Are the Psychologists Credentialing Requirements?
Additional requirements:
- Doctoral degree (PhD, PsyD, EdD in Psychology) , official transcript
- State psychology license , copy + verification from state board
- Internship and postdoctoral training documentation
- APA accreditation confirmation (if applicable)
- Neuropsychological testing credentials (if billing for testing services)
Frequent mistake: Submitting training documentation that doesn’t clearly list supervised hours or the name of the supervising psychologist. Payers often reject incomplete training verification.
Enrollment challenge: Psychologists seeking Medicare enrollment must complete PECOS (Provider Enrollment, Chain, and Ownership System) separately from commercial credentialing.
What Are the Credentialing Requirements for Psychiatrists?
Additional requirements:
- Medical degree (MD or DO)
- Residency completion letter , psychiatry specialty
- Board certification in psychiatry (ABPN) , or board eligibility documentation
- DEA registration (active, current state)
- Hospital privileges documentation (if applicable)
- Controlled substance license for state of practice
Frequent mistake: Allowing DEA registration to lapse between the credentialing application and payer approval. DEA expiration during the review period triggers an automatic hold.
Enrollment challenge: Psychiatrists credentialing with MBHO carve-outs (Optum Behavioral Health, Carelon) must complete a separate enrollment distinct from the base commercial plan. Many assume credentialing with Aetna covers Aetna Behavioral Health , it often does not.
What Are the Credentialing Requirements for LCSWs?
Additional requirements:
- Master’s degree in social work (MSW) , transcript
- LCSW license , current, state-specific
- Clinical supervised hours documentation (typically 3,000 hours post-MSW for LCSW)
- Supervisor verification letter (some payers require this)
Frequent mistake: Submitting LMSW (Licensed Master Social Worker) credentials when LCSW is required. Most payers only credential LCSWs for independent practice , not pre-licensure designations.
Enrollment challenge: LCSW scope of practice varies by state. Payers operating in multiple states apply different enrollment rules based on the state of licensure, not the state of practice. Verify payer rules state-by-state.
What Are the Credentialing Requirements for LMHCs and LPCs?
Additional requirements:
- Master’s degree in counseling or related field , transcript
- State license (LMHC, LPC, LCPC , varies by state)
- Supervised clinical hours documentation , typically 2,000–3,000 post-degree hours
- State-specific exam confirmation (NCE, NCMHCE)
Frequent mistake: Submitting a license with a suffix not recognized by the target payer. License title varies widely by state (LPC in Texas, LPCC in California, LCMHC in North Carolina). Payers verify against their approved designation list.
Enrollment challenge: Some commercial payers and Medicare do not credential LMHCs/LPCs for independent billing in certain states. Verify payer-specific eligible provider lists before beginning enrollment.
Credentialing Is Just One Piece. Here's the Full Operational Picture.
The Behavioral Health Operations Playbook covers credentialing workflows, billing best practices, RCM KPIs, and denial prevention , everything a behavioral health practice needs to run efficiently from day one.
What Are the Credentialing Requirements for LMFTs?
Additional requirements:
- Master’s or doctoral degree in marriage and family therapy , transcript
- LMFT license , current and state-specific
- Supervised clinical hours (2,000–4,000 hours depending on state)
- AAMFT membership (some payers request this; not universally required)
Frequent mistake: Assuming LMFT credentialing status transfers across state lines. If a therapist is licensed in multiple states, each state license requires separate credentialing with each payer in that state.
Enrollment challenge: LMFTs often face the longest credentialing timelines of the outpatient therapy licenses , particularly with Medicaid managed care organizations, which have their own enrollment processes separate from commercial payer credentialing.
What Are the Credentialing Requirements for Psychiatric Nurse Practitioners?
Additional requirements:
- RN license , current
- APRN/NP license , current, with psychiatric-mental health specialty designation
- Board certification , PMHNP-BC (ANCC)
- Prescriptive authority documentation , state-specific
- DEA registration (active)
- Collaborative agreement (if required by state)
- National certification copy
Frequent mistake: Not disclosing a collaborative agreement requirement when states require physician oversight. Payers that require collaborative agreements will hold enrollment until this documentation is complete.
Enrollment challenge: PMHNPs are among the fastest-growing behavioral health provider types , but payer credentialing departments are inconsistent in how they classify them. Some payers credential PMHNPs under nursing; others under behavioral health. Routing applications to the wrong department adds weeks.
What Are the Credentialing Requirements for BCBAs and ABA Therapists?
Additional requirements:
- BCBA certification , current and active (BACB-verified)
- Master’s degree (for BCBA) , transcript
- State licensure (where applicable , LBA, LABA)
- Supervised hours documentation for RBT and BCaBA levels (if billing at those levels)
- ABA-specific payer credentialing application (many payers have specialty-specific forms)
Frequent mistake: BCBAs attempting to credential through standard behavioral health pathways when the payer has a separate ABA credentialing process. Most major payers (Optum, Cigna, Aetna) have dedicated ABA credentialing departments distinct from general behavioral health.
Enrollment challenge: ABA billing has unique authorization and billing requirements , H2019 (behavior intervention), H0032 (therapy assessment), and specific modifier requirements , that differ from outpatient therapy. Credentialing and billing expertise must align.
What Are the Credentialing Requirements for Substance Abuse Counselors?
Additional requirements:
- Addiction counseling credentials , CADC, LADC, LCDC, CAC (title varies by state)
- State-specific licensure (LAC, LPC-A, LCAS , varies significantly)
- Clinical supervised hours documentation
- NAADAC membership or certification (some payers request)
Frequent mistake: Attempting to credential with commercial plans before confirming the counselor’s credential level meets the payer’s minimum requirement. Many commercial payers require LCDC or equivalent , not CADC.
Enrollment challenge: Substance abuse counselors credentialing with MBHOs for SUD treatment programs face an additional layer , OTP (Opioid Treatment Program) certification for methadone providers, and SAMHSA certification for certain SUD treatment facilities.
What Are the Additional Credentialing Requirements for Group Practices?
Group practices have all individual provider requirements, plus:
- ✅ Group NPI (Type 2) , registered and active
- ✅ Group Tax ID (EIN) , W-9 with group entity information
- ✅ Group practice payer enrollment , separate from individual provider enrollment
- ✅ Business license , state-specific
- ✅ Organizational NPI linked to each rendering provider’s individual NPI
- ✅ Facility accreditation (if applicable , CARF, Joint Commission)
- ✅ Group credentialing application submitted alongside (or before) individual provider applications
Critical rule: At most payers, individual provider credentialing and group enrollment are two separate processes. A provider can be individually credentialed but unable to bill under the group NPI until group enrollment is also approved. Both must be active before claims submit correctly.
What Are the Most Common Credentialing Mistakes That Cause Delays?
These are the errors that add weeks , or months , to the process:
- Incomplete CAQH profile , Missing sections, outdated documents, or expired attestation dates are the top cause of payer-side credentialing holds. CAQH re-attestation is required every 120 days.
- License expiration during the review period , A license that expires between application submission and payer approval can restart the entire review.
- Malpractice coverage gaps , Any gap in malpractice coverage history , even one day , triggers additional review.
- CV gaps unexplained , Any gap in work history over 30 days requires a written explanation. Leaving gaps blank generates a hold.
- Wrong license type submitted , Submitting LMSW when payer requires LCSW, or submitting pre-licensure credentials for a payer that only accepts fully licensed providers.
Not tracking application status , Most payers do not proactively notify providers of missing items. Follow-up at day 30, 60, and 90 is required to keep applications moving.
How Long Does Behavioral Health Credentialing Take and How Do You Speed It Up?
| Payer Type | Typical Timeline |
|---|---|
| Commercial payers (Aetna, Cigna, BCBS) | 60–90 days |
| MBHO carve-outs (Optum, Carelon, Magellan) | 90–120 days |
| Medicare (PECOS) | 60–90 days |
| Medicaid (state-specific) | 90–180 days |
| ABA specialty credentialing | 90–150 days |
How to accelerate the timeline:
- Submit a complete, error-free application on the first submission
- Have CAQH fully completed and attested before applications go out
- Follow up with every payer at day 30, day 60, and day 90
- Track every application in a centralized system with submission date, status, and next follow-up date
- Begin credentialing at hire , not after orientation is complete
Wrong Document. Wrong License Type. One Mistake Delays Everything.
Credentialing errors don’t announce themselves , they show up as delayed approvals and unbilled sessions 90 days later. BehavioralProz ensures every application is complete, correct, and actively followed up on.
Frequently Asked Questions
How long does behavioral health credentialing take?
Commercial payers typically take 60–90 days; MBHO carve-outs (Optum, Carelon) take 90–120 days; Medicaid can take 90–180 days depending on the state.
What documents are required for behavioral health credentialing?
Every provider needs an active NPI, completed CAQH profile, current state license, malpractice certificate, CV with no unexplained gaps, education transcripts, and a signed payer application.
What is CAQH and why is it required for credentialing?
CAQH ProView is a centralized credentialing database used by most commercial payers. Providers must complete and attest their profile every 120 days , an incomplete or expired profile pauses credentialing at every payer simultaneously.
Can a therapist see patients before credentialing is complete?
Yes, but only as out-of-network. Until credentialing is approved, the provider cannot bill at in-network rates , meaning patients pay full out-of-pocket fees or the practice absorbs the reimbursement gap.
Do group practices need separate credentialing from individual providers?
Yes. Individual provider credentialing and group practice enrollment are separate processes. Both must be approved before claims can be submitted under the group NPI.
What is the most common reason behavioral health credentialing gets delayed?
Incomplete or outdated CAQH profiles are the top cause, followed by unexplained CV gaps, expired malpractice certificates, and failure to follow up with payers at regular intervals.
Do LMFTs and LPCs qualify for insurance credentialing?
Yes, but eligibility varies by payer and state. Some commercial plans and Medicare do not credential LMFTs or LPCs for independent billing in certain states. Verify each payer’s eligible provider list before applying.

