Table of Contents
How Medicaid Cuts Disrupt ABA Practices in 2026
What if everything you’ve worked so hard for your ABA Practice management, your scheduling for your team, your billing processes was suddenly not enough? Medicaid cuts are no longer an issue of what is to come, it’s already at your doorstep disrupting the core of ABA (Applied Behavioral Analysis) care delivery and your billing processes.
The “One Big Beautiful Bill Act” (OBBBA), a detailed legislative bill that was signed on July 4, 2025, aims to streamline Medicaid spending, which includes heavy cuts specifically targeting ABA therapy funding.
The Medicaid cuts are a true threat to ABA practices that is more than a matter of shrinking revenue. It is a problem of how you continue to provide consistent quality care to the children and families that need you while operating in a risk environment of changing Medicaid regulations.
The ABA therapists are being forced to think of how to operate as the Medicaid cuts are already in force. What has worked up until now will no longer be effective. You’re going to see diminished therapy hours, stricter eligibility standards and intimidating increased ABA audit therapy risks and claim denials.
And it’s not just your ABA practice management put to the test – it’s your patients, your staff, and the mission that drives your work every day.
Through this blog, let us help you to have a clear understanding of the regulatory changes that are the cause of the Medicaid changes, how to identify high risk areas in your billing processes and how to revise your protocols, appeals and documentation for higher reimbursements.
Why Medicaid Funding Matters for ABA Therapy Providers?
“Medicaid plays a key role in helping people with autism and their families access the care and support they need throughout their lives”, Angela Lello, Senior Director for Public Policy.
Medicaid, once a lifeline for millions of poor families, is under legitimate pressure from federal and state budgets to cut and reshape reimbursement policies.
Your ABA therapy hours are being cut, eligibility requirements tightened, and audits risks heightened, sometimes cutting care to 30 hours per week per child and just a temporary length of time.
As an ABA provider, you may be wondering how these Medicaid reductions are going to affect your Medicaid-reliant families, your treatment staff, and your bottom line.
ABA Practices that rely on Medicaid funding are already feeling the pressure of longer waiting lists, gaps in treatment, and diminishing margins.
You might have to face more ABA therapy claim denials, lesser reimbursement rates, and increased ABA compliance requirements. Now ABA Therapy revenue cycle management must be stringent with proper billing, precise medical coding, and proper documentation which is crucial to maintain your practice uninterrupted.
Why ABA Providers Must Act Fast on Medicaid Cuts?
The 2025 Medicaid cuts are redoing how your ABA practice operates, provides care, and manages revenue, with instant, measurable consequences.
The “One Big Beautiful Bill Act” reduced Medicaid spending by more than $1 trillion and required ABA clinics to implement instant coverage, reimbursement, and staffing cuts. All staffing, scheduling, and billing decisions as an ABA provider now have greater risk.
“Along with the Medicaid cuts, and other provisions making it harder for people to enroll in ACA plans even when eligible, the Congressional Budget Office estimates that the total number of uninsured will rise by
17 million people by 2034
.” Said William Dow, professor of health policy and management at UC Berkeley School of Public Health and director of the Center on the Economics and Demography of Aging
At the national level, Medicaid therapy limits (30 hours/week for three years) impose actual limits on care to each individual child, and millions of Americans are at risk of losing Medicaid altogether, with increased wait lists, tightened eligibility, and increased denial rates.
Practice is facing revenue reduction, payment delay, and need to re-imagine workflows, so it must be agile and ahead of the game.
If Medicaid income in your clinic represents 60% or more of gross revenue, the effect is now and it’s severe. It’s time to project billing, examine denial management, and protect margins before the financial strain constricts further.
Key OBBBA Policy Shifts Impacting ABA Providers
Key policy changes enacted through H.R. 1 are going to redefine how Medicaid supports ABA services. The provisions significantly affect funding, operations, and continuity of care. Here’s the breakdown of the four most significant changes, and what they mean to your practice.

1. How Federal Spending Caps Threaten ABA Funding?
H.R. 1 proposes caps on federal funding to Medicaid in terms of population or as block grants. This is a significant departure from the existing model, under which federal funding is based on medical costs and demand.
Implications for ABA providers
This change can result in states having fewer funds in the long term, since care costs will increase. The bill pushes the best-performing states into possibly cutting therapy hours, tightening eligibility, and reducing reimbursement rates. ABA providers can expect decreased access and diminishing margins.
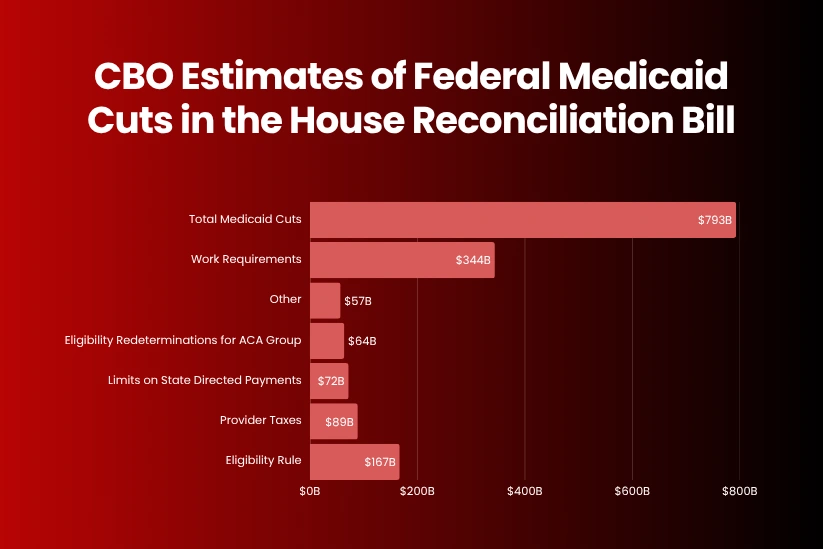
The Congressional Budget Office’s (CBO) latest cost estimate shows that the bill would reduce federal Medicaid spending by $793 billion and that the Medicaid provisions would increase the number of uninsured people by 7.8 million.
On August 1, 2025, the Nebraska Department of Health and Human Services cut the reimbursement rates for ABA Therapy to around 48%, which lowered the Medicaid funding.
2. How the Provider Tax Freeze Tightens Medicaid Budgets?
The bill would put current state provider taxes, which are often used to help fund Medicaid, into hold at current levels, when the bill goes into effect. It also prohibits states from adjusting such taxes or imposing new ones in the future.
Impact on ABA practice management
States stand to lose as much as $16 billion in optional Medicaid funding each year. To compensate for the loss, many of them would have to cut physician payment rates or revert enrollment, directly affecting how much your practice is reimbursed for services delivered.
3. Will 6-Month Checks Disrupt ABA Medicaid Coverage?
In 2026, “able-bodied” Medicaid beneficiaries will be required to meet work requirements and be redetermined for eligibility every six months (instead of every 12 months) from the current annual process.
What this means for ABA Therapy Providers:
While the policies impact adult beneficiaries, they impose broad administrative burdens. ABA therapy providers must anticipate delays in authorization, more paperwork, and the possibility of disrupted service, particularly for ABA client families that risk losing coverage due to missing deadlines or becoming mired in red tape.
4. How State Payment Cuts Affect ABA Reimbursements
H.R. 1 also aims at state-directed payments, may reduce or phase out supplemental funds used by states to support increased reimbursement rates for particular providers or services.
For ABA providers:
If your clinic is being paid additional for supervision by BCBA, specialized personnel, or regional wage adjustment, those funds may be phased out. This could affect your ability to recruit, retain, and equitably pay qualified staff, thereby impacting sustainability of care.
What Your ABA Practice Needs to Do Now
Although the Early and Periodic Screening, Diagnostic and Treatment (EPSDT) mandate continues to shield medically necessary autism services for children through age 21, the fiscal and operational environment is changing. To remain on top of the situation:
- Assess your fiscal exposure to Medicaid reimbursement
- Enhance billing systems and denial management systems
- Consider payer diversification and commercial contracting strategies
- Re-assess staff and service models for long-term viability
Proactive planning now is the best insurance against loss of access to care, and disruption of income, to ensure your practice is equipped to anticipate the changing Medicaid landscape.
How ABA Providers Can Stay Resilient Amid Medicaid Cuts
- Policy Pressure Points: Get a clear view of national and state-level caps on therapy hours, lower reimbursement rates, and decreased Medicaid eligibility standards already impacting ABA coverage.
- Operational Impact in Real Time: See how these events impact patient intake, staffing issues, and cash flow in real time, compelling many practices to reframe their business today, not tomorrow.
- Must-Know Facts: Monitor key figures, such as 7.6 million Americans who are at risk of losing Medicaid benefits and state ABA reimbursement cuts up to 48%.
- Pro Tips for Billing & Medicaid Compliance: Discover smart, practical tips to further refine medical coding, maximize billing precision for Medicaid and commercial payers, and increase denial management success.
- Tech-Driven Solutions & Strategic Partners: Find technology-driven solutions and professional RCM partners like Behavioral Proz specializing in ABA billing, appeals, and reimbursement recovery.
Why It’s Time to Rethink ABA Medicaid Billing
- Rigid Billing Systems: Billing tactics created for stable reimbursement now battle denials due to caps and eligibility modifications.
- Revenue Susceptibility: Fee-for-service models with volume-based fees and commodity pricing are shrinking under lowered rates and volume limitations.
- Increased Pressure for Medicaid Compliance: The ongoing demand for detailed clinical documentation, support for treatment, and specific outcome data is placing a burden on older practice management systems, risking delayed payment or clawback.
- Changing Policies at an Accelerated Pace: Without constant monitoring and communication with payers, practices cannot keep up with new rules and audit requirements.
2026 Medicaid Cuts: How Much Revenue Is at Risk?
- Increased enrollment and coverage instability
- Increased administrative workload
- Increased complexity in billing and tracing eligibility
- Pressure on revenue cycle management and care continuity
Top 3 Challenges for ABA Providers Under Medicaid Cuts
Therapy Hour Limits and Eligibility Restrictions
One of the biggest challenges that ABA therapies are going to have is imposing severe therapy hour limits and stricter Medicaid standards. In some states such as Indiana and California, recent policies limit ABA services to 30 hours a week, usually with a maximum duration of three years.
For clients, it disrupts regular care and breaks momentum. For your staff, it creates difficult decisions about how to allocate limited hours among clients with more needs.
And for your practice? It has the potential to harm patient retention rates, lower revenues, and close margins, particularly if Medicaid dominates your payer mix.
And, as a reality, some states are seeing 20–30% decreases in billable hours of therapy that have a direct impact on the bottom line.
Increased Scrutiny and Claim Denials in Billing
With the 2025 Medicaid updates, billing audits and documentation reviews are increasing nationwide. Regulators are acting in response to previous overpayment problems, such as the $56 million in improper payments identified in Indiana, by closing
loopholes and tightening scrutiny.
According to the 2024 OIG report, at least $56 million improper ABA payments are made in Indiana, citing problems with documentation, diagnostic evaluations, staff credentials, referrals and more.
With the Medicaid cuts, now you’re likely dealing with:
- More pre-authorizations
- Tighter documentation standards
- Higher ABA therapy claim denial rates (up to 30%) for some ABA claims
Every delayed or denied claim puts more strain on your revenue cycle. And for smaller practices without large billing teams, this administrative burden can pull attention away from clinical care.
Workforce Shortages and Operational Inefficiencies
Medicaid reductions compound current workforce issues in ABA treatment. As dollars pay out, typically as much as 50%, your practice struggles to provide competitive pay and keep quality therapists on staff.
Staff turnover and clinician burnout rates increase as operating inefficiencies accumulate under the stress of more administrative tasks, stricter documentation rules, and uncertainty regarding funding viability.
The Domino Effect Of These Challenges
These challenges tend to overlap, amplify their impact and put serious pressure on your ABA practice. When therapy hour caps cut into your billable services and Medicaid rates drop, your revenue takes a hit.
Meanwhile, increased ABA therapy claims denials and delayed payments skim cash flow, making it difficult to retain staff, provide competitive salaries, or invest in equipment that streamlines billing precision.
With increased administrative overhead of rules of ABA compliance, you will experience increasing cost of operation and diminishing time for clinical practice.
Altogether, it is a tense environment where maintaining your doors open and providing quality care is a daily juggling act.
It’s the time now to examine your billing practices, denial management processes, and staffing plans, before these challenges lead to service cuts or even practice closure.
Is Your ABA Billing Ready to Withstand Medicaid Cuts?
Is Your ABA Billing Audit-Ready? Ask yourself these Questions:
- Are session notes comprehensive enough to pass state Medicaid documentation requirements?
- Do CPT codes reflect the service rendered and clinician’s qualifications accurately?
- Are all modifiers for services current and properly utilized?
- Do you scrutinize medical necessity documentation prior to billing?
- Are pre-authorization requests submitted and monitored regularly?
- Do you have a method for alerting authorization lapse or hour thresholds?
- Are denial causes coded and used to simplify workflows?
- Is your billing staff getting ongoing education on Medicaid policy updates?
- Is there a formal procedure for answering payer audits or information requests?
- Do you report underpayments or silent write-offs in your reports?
5 Proven Ways to Prepare Your ABA Practice for Medicaid Cuts in 2026:
Rather than waiting for policy change to happen in earnest, it makes sense to deliberately be ahead of the curve. Here’s how to do it:Strengthen Your Billing Structure:
Whether this takes the form of in-house billing or outsourced, now is the time to stress test your system.- Audit your workflow periodically
- Educate your staff on new Medicaid regulations
- Catch documentation gaps early
Rethink Revenue Strategy
If you rely heavily on Medicaid reimbursements, you are open to policy risk.- Introduce private pay tiers or hybrid plans
- Seek contracts with commercial insurers or local school districts
- Apply for autism-focused grants or county funds
- Offer parent training programs as an add-on service
Build a Denial-Resistant Culture
Denials are increasing and often have little to do with quality, but everything to do with paperwork.- Track denial trend analysis in real time
- Standardize documentation templates
- Create appeal SOPs (Standard Operating Procedures)
- Establish denial response KPIs for your billing team
Stay Sharp with Evolving Medical Coding
Even minor CPT or modifier mistakes can trigger flags on your claims.- Subscribe to CPT update-alerts
- Train staff quarterly on coding changes
- Retain a reference sheet for all frontline staff
Advocate Strategically
You’re not powerless, provider voices make a difference.- Join ABA provider partnerships or local task forces
- Document how proposed cuts impact your clients
- Engage parents/guardians and caregivers in grassroots advocacy
Major 2026 Medicaid Policy Changes for ABA Providers
From the beginning of 2026, several major federal policy changes will reshape how Medicaid is administered, impacting both patient access and provider operations.
| Effective Date | Policy Update | Summary & Implications |
|---|---|---|
| Jan 1, 2026 | Expiration of Enhanced FMAP | The enhanced Federal Medical Assistance Percentage (FMAP), which has supported Medicaid expansion under the Affordable Care Act, is set to expire. This federal match, covering up to 90% of costs for newly eligible adults, has enabled many states to expand coverage over the past decade. Without it, states will face significantly higher Medicaid costs, likely prompting reduced benefits, restricted eligibility, and greater financial strain on providers. |
| Oct 1, 2026 | Restricted Eligibility for Non-Citizens | Eligibility criteria will narrow for some non-U.S. citizens, potentially reducing Medicaid enrollment among vulnerable populations. Providers should anticipate coverage disruptions and increased administrative workload related to eligibility verification and service continuity. |
| Dec 31, 2026 | Semi-Annual Eligibility Redeterminations | All states will be required to assess Medicaid eligibility changes every six months, rather than annually. While intended to improve oversight, this shift will likely result in increased coverage loss, often due to administrative barriers, affecting even individuals who still meet eligibility criteria. Practices should prepare for greater patient churn and potential service gaps. |
| Jan 1, 2027 | Implementation of Work Requirements | Most adult Medicaid beneficiaries will be required to demonstrate 80 hours per month of employment, education, or volunteer activity to maintain coverage. Exemptions will apply for children, seniors, primary caregivers, tribal members, and individuals deemed medically frail. The Congressional Budget Office estimates this policy will reduce federal Medicaid spending by over $325 billion in ten years. However, evidence from previous state-level implementations shows minimal employment impact and significant coverage losses, particularly among individuals already working or managing health conditions. |
| Oct 1, 2028 | Cost Sharing + Provider Tax Limits | States will be required to introduce cost-sharing mechanisms for certain Medicaid-covered services. Exceptions include primary care, behavioral health, and services provided by FQHCs, CCBHCs, and RHCs. Additionally, new limits on provider tax rates may constrain how states fund their Medicaid programs, increasing the likelihood of rate cuts or service reductions. |
3 Steps to Tackle Medicaid Cuts and Stay Profitable
Assess Your Risk
- Determine how much of your revenue relies on Medicaid reimbursement rate and identify which states are most vulnerable.
- Audit your recent claims: focus on denials, discrepancies, and proper use of ABA therapy CPT codes and modifiers.
- Educate everyone, clinicians, billers, admin, on policy changes, documentation standards, and ABA compliance updates.
- Stay ahead: subscribe to state Medicaid updates and track changes that affect your practice.
Strengthen Operational Systems
- Rework authorizations and scheduling to adapt to hour caps while still offering effective treatment.
- Build or refine your denial management process so rejections don’t go unanswered.
- Check if your ABA billing software or EHR is optimized for ABA—look for error prevention and workflow efficiency.
- Consider tapping experts, revenue cycle management (RCM) services with ABA experience can add value fast.
Fix, Embed & Future-Proof
- Roll out RCM tools and expert protocols into your daily workflow.
- Redo your financial projections and budgets based on Medicaid reductions and operational shifts.
- Align your clinical, billing, and admin teams to work together on ABA compliance requirements and strategy.
- Strengthen relationships: talk with Medicaid officials, join advocacy efforts, and let your voice be heard.
Medicaid Cuts in 2026: How Will Your ABA Practice Respond?
Medicaid cuts present a real challenge, but also a call to action. Technology integration, proactive billing management, and workforce agility stand as pillars of success in 2025 and beyond.
What does this mean for your ABA practice? The future will reward those who anticipate change and act decisively, leveraging data, technology, and expert partners to safeguard financial health while continuing to deliver life-changing therapy.
Start today by conducting a thorough Medicaid revenue and billing review to identify risks and opportunities. Then, consider engaging specialized revenue cycle management resources familiar with ABA, such as Behavioral Proz, to support Medicaid compliance and reimbursement.
How is your practice preparing to meet the Medicaid challenges ahead? Taking early, informed action will determine your ability to sustain care excellence and financial stability.








